Preparing for the inevitable earthquake risk in Dhaka: A physiatrist’s perspective
Authors
- Md. Israt HasanDepartment of Physical Medicine and Rehabilitation, Sher-E-Bangla Medical College, Barishal, Bangladesh
- Fatema NewazDepartment of Physical Medicine and Rehabilitation, Kumudini Women’s Medical College, Tangail, Bangladesh
- Syed Mozaffar AhmedDepartment of Physical Medicine and Rehabilitation, Bangladesh Medical University, Dhaka, Bangladesh
DOI:
Keywords
Downloads
Correspondence
Publication history
Responsible editor
Reviewers
Funding
Ethical approval
Trial registration number
Copyright
Published by Bangladesh Medical University (former Bangabandhu Sheikh Mujib Medical University).
Dhaka, a densely populated megacity, faces a real and potentially catastrophic earthquake risk. Even moderate earthquakes have caused fatalities, highlighting vulnerability to larger events. Unplanned urbanization, vulnerable infrastructure, and seismic proximity increase its risk of mass casualties. Studies show low seismic risk perception and inadequate household preparedness, revealing critical gaps in public awareness and institutional readiness [1]. Bangladesh’s disaster preparedness focuses on mortality reduction and emergency response, with limited attention to injury, disability, and long-term functional loss, reflecting a critical deficiency from a physiatrist’s perspective. This study examines the rehabilitation preparedness in Dhaka and proposes a practical, physiatrist-led framework for integrating rehabilitation into disaster response. Recent earthquakes in and around Dhaka (2017–2025), including moderate events up to magnitude 6.2 with reported deaths, injuries, and structural damage, demonstrate ongoing seismic activity and highlight the city’s vulnerability, although these events do not represent probabilistic risk projections.
Geographically, Bangladesh lies close to the Indian–Eurasian plate boundary, with several active fault systems capable of producing large earthquakes. Seismological data indicate that Dhaka is at risk from both distant major events and moderate-to-severe earthquakes originating near or beneath the city. In this context, earthquake impacts extend far beyond immediate mortality. Evidence from global disasters shows that many survivors sustain fractures, spinal cord and traumatic brain injuries, crush injuries, amputations, and soft-tissue trauma, leading to substantial long-term disability without early rehabilitation. Although Bangladesh-specific data are limited, findings from disaster-affected settings such as the 2017 Bangladesh landslide indicates substantial unmet rehabilitation needs and system constraints [2]. Similar patterns are likely in Dhaka due to urban and health system vulnerabilities, which may overwhelm response and, without integrated rehabilitation, convert survivable injuries into long-term disability [3].
Physiatry plays a central yet often overlooked role in disaster response. Physiatrists focus on function, independence, and participation beyond the acute phase of injury [4]. In disaster settings, physiatrists serve as team leaders, multidisciplinary coordinators, policy advocates, and liaisons between acute care and long-term functional recovery. Early rehabilitation during acute care reduces complications and, as demonstrated in earthquakes in Nepal and Türkiye, improves functional outcomes and reduces long-term disability. Key interventions including mobilization, positioning, pain management, and timely provision of assistive devices further enhance recovery [5]. Without physiatrist-led coordination, these opportunities are often missed.
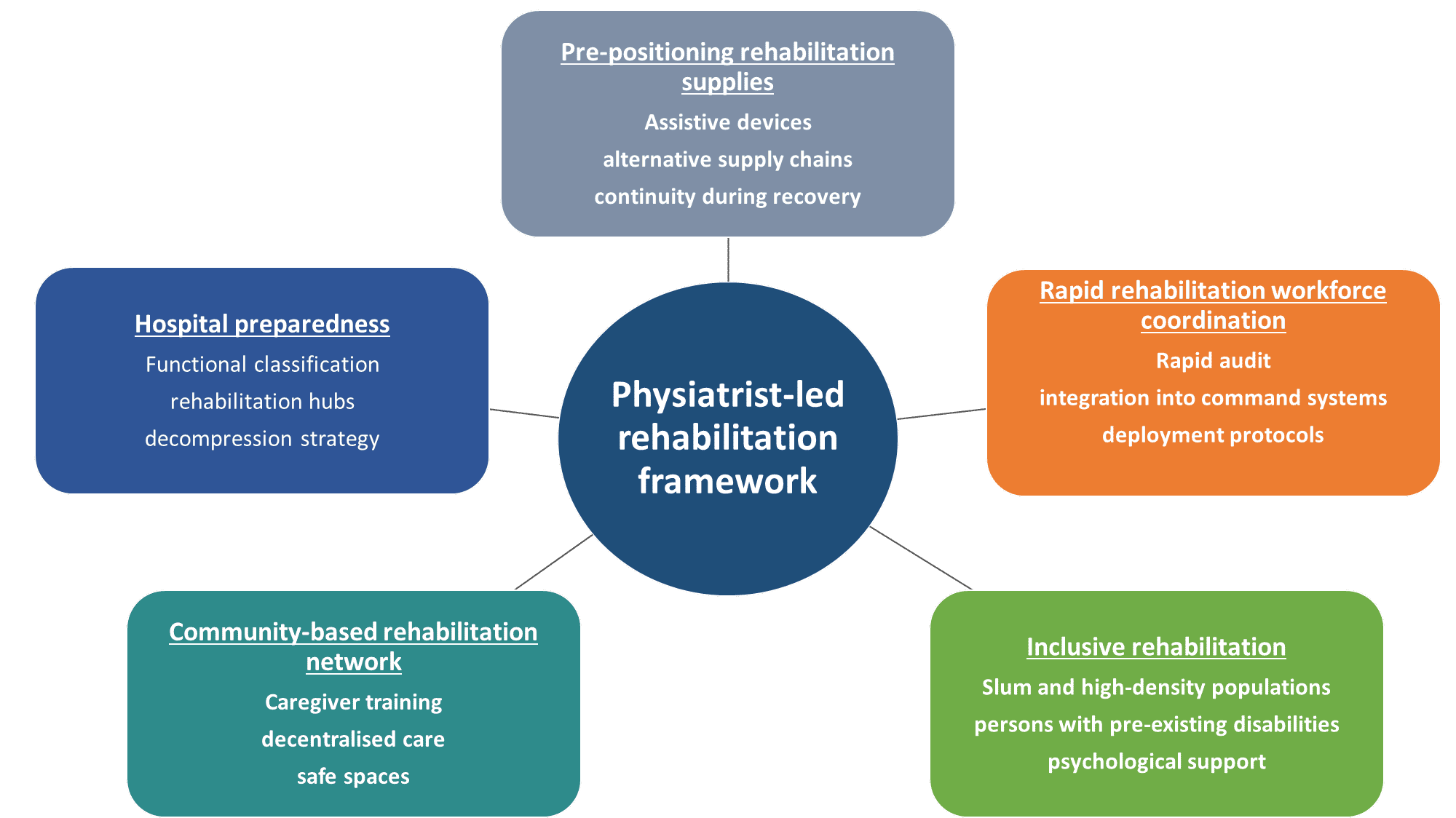
Figure 1 Physiatrist-led rehabilitation preparedness framework for earthquake response in Dhaka
Equally concerning is the vulnerability of people with pre-existing disabilities. Individuals who depend on wheelchairs, prostheses, orthoses, or caregivers face heightened risks of injury, displacement, and loss of independence during earthquakes. Disaster preparedness plans seldom address accessible evacuation, continuity of rehabilitation care, or replacement of assistive devices, contradicting principles of disability-inclusive disaster risk reduction and further marginalizing this population.
Integrating rehabilitation into national disaster policies and emergency medical team frameworks is essential for system-level implementation. As a major earthquake in Dhaka remains inevitable, preparedness must address the predictable surge of disability. A physiatrist-led approach can reduce suffering and support resilient, function-focused health systems.


Variables | Frequency (%) |
Indication of colposcopy |
|
Visual inspection of the cervix with acetic acid positive | 200 (66.7) |
Abnormal pap test | 13 (4.3) |
Human papilloma virus DNA positive | 4 (1.3) |
Suspicious looking cervix | 14 (4.7) |
Others (per vaginal discharge, post-coital bleeding) | 69 (23.0) |
Histopathological diagnosis | |
Cervical Intraepithelial Neoplasia 1 | 193 (64.3) |
Cervical Intraepithelial Neoplasia 2 | 26 (8.7) |
Cervical Intraepithelial Neoplasia 3 | 32 (10.7) |
Invasive cervical cancer | 27 (9.0) |
Chronic cervicitis | 17 (5.6) |
Squamous metaplasia | 5 (1.7) |
Groups based on pre-test marks | Pretest | Posttest Marks (%) | Difference in pre and post-test marks (mean improvement) | P |
Didactic lecture classes | ||||
<50% | 36.6 (4.8) | 63.2 (9.4) | 26.6 | <0.001 |
≥50% | 52.8 (4.5) | 72.4 (14.9) | 19.6 | <0.001 |
Flipped classes | ||||
<50% | 36.9 (4.7) | 82.2 (10.8) | 45.4 | <0.001 |
≥50% | 52.8 (4.6) | 84.2 (10.3) | 31.4 | <0.001 |
Data presented as mean (standard deviation) | ||||
Background characteristics | Number (%) |
Age at presentation (weeks)a | 14.3 (9.2) |
Gestational age at birth (weeks)a | 37.5 (2.8) |
Birth weight (grams)a | 2,975.0 (825.0) |
Sex |
|
Male | 82 (41) |
Female | 118 (59) |
Affected side |
|
Right | 140 (70) |
Left | 54 (27) |
Bilateral | 6 (3) |
Delivery type |
|
Normal vaginal delivery | 152 (76) |
Instrumental delivery | 40 (20) |
Cesarean section | 8 (4) |
Place of delivery |
|
Home delivery by traditional birth attendant | 30 (15) |
Hospital delivery by midwife | 120 (60) |
Hospital delivery by doctor | 50 (25) |
Prolonged labor | 136 (68) |
Presentation |
|
Cephalic | 144 (72) |
Breech | 40 (20) |
Transverse | 16 (8) |
Shoulder dystocia | 136 (68) |
Maternal diabetes | 40 (20) |
Maternal age (years)a | 27.5 (6.8) |
Parity of mother |
|
Primipara | 156 (78) |
Multipara | 156 (78) |
aMean (standard deviation), all others are n (%) | |
Background characteristics | Number (%) |
Age at presentation (weeks)a | 14.3 (9.2) |
Gestational age at birth (weeks)a | 37.5 (2.8) |
Birth weight (grams)a | 2,975.0 (825.0) |
Sex |
|
Male | 82 (41) |
Female | 118 (59) |
Affected side |
|
Right | 140 (70) |
Left | 54 (27) |
Bilateral | 6 (3) |
Delivery type |
|
Normal vaginal delivery | 152 (76) |
Instrumental delivery | 40 (20) |
Cesarean section | 8 (4) |
Place of delivery |
|
Home delivery by traditional birth attendant | 30 (15) |
Hospital delivery by midwife | 120 (60) |
Hospital delivery by doctor | 50 (25) |
Prolonged labor | 136 (68) |
Presentation |
|
Cephalic | 144 (72) |
Breech | 40 (20) |
Transverse | 16 (8) |
Shoulder dystocia | 136 (68) |
Maternal diabetes | 40 (20) |
Maternal age (years)a | 27.5 (6.8) |
Parity of mother |
|
Primipara | 156 (78) |
Multipara | 156 (78) |
aMean (standard deviation), all others are n (%) | |
Mean escape latency of acquisition day | Groups | ||||
NC | SC | ColC | Pre-SwE Exp | Post-SwE Exp | |
Days |
|
|
|
|
|
1st | 26.2 (2.3) | 30.6 (2.4) | 60.0 (0.0)b | 43.2 (1.8)b | 43.8 (1.6)b |
2nd | 22.6 (1.0) | 25.4 (0.6) | 58.9 (0.5)b | 38.6 (2.0)b | 40.5 (1.2)b |
3rd | 14.5 (1.8) | 18.9 (0.4) | 56.5 (1.2)b | 34.2 (1.9)b | 33.8 (1.0)b |
4th | 13.1 (1.7) | 17.5 (0.8) | 53.9 (0.7)b | 35.0 (1.6)b | 34.9 (1.6)b |
5th | 13.0 (1.2) | 15.9 (0.7) | 51.7 (2.0)b | 25.9 (0.7)b | 27.7 (0.9)b |
6th | 12.2 (1.0) | 13.3 (0.4) | 49.5 (2.0)b | 16.8 (1.1)b | 16.8 (0.8)b |
Average of acquisition days | |||||
5th and 6th | 12.6 (0.2) | 14.6 (0.8) | 50.6 (0.7)b | 20.4 (2.1)a | 22.4 (3.2)a |
NC indicates normal control; SC, Sham control; ColC, colchicine control; SwE, swimming exercise exposure. aP <0.05; bP <0.01. | |||||
Categories | Number (%) |
Sex |
|
Male | 36 (60.0) |
Female | 24 (40.0) |
Age in yearsa | 8.8 (4.2) |
Education |
|
Pre-school | 20 (33.3) |
Elementary school | 24 (40.0) |
Junior high school | 16 (26.7) |
Cancer diagnoses |
|
Acute lymphoblastic leukemia | 33 (55) |
Retinoblastoma | 5 (8.3) |
Acute myeloid leukemia | 4 (6.7) |
Non-Hodgkins lymphoma | 4 (6.7) |
Osteosarcoma | 3 (5) |
Hepatoblastoma | 2 (3.3) |
Lymphoma | 2 (3.3) |
Neuroblastoma | 2 (3.3) |
Medulloblastoma | 1 (1.7) |
Neurofibroma | 1 (1.7) |
Ovarian tumour | 1 (1.7) |
Pancreatic cancer | 1 (1.7) |
Rhabdomyosarcoma | 1 (1.7) |
aMean (standard deviation) | |



Test results | Disease | Sensitivity (%) | Specificity (%) | PPV (%) | NPV (%) | ||
Yes | No | ||||||
Reid’s score ≥ 5 | Positive | 10 | 15 | 37.0 | 94.5 | 40.1 | 93.8 |
Negative | 17 | 258 |
|
|
|
| |
Swede score ≥ 5 | Positive | 20 | 150 | 74.1 | 45.0 | 11.8 | 94.6 |
Negative | 7 | 123 |
|
|
|
| |
Swede score ≥ 8 | Positive | 3 | 21 | 11.1 | 92.3 | 12.5 | 91.3 |
Negative | 24 | 252 |
|
|
|
| |
a High-grade indicates a score of ≥5 in both tests; PPV indicates positive predictive value; NPV, negative predictive value | |||||||
Test | Sensitivity (%) | Specificity (%) | Positive predictive value (%) | Negative predictive value (%) |
Reid’s score ≥ 5 | 37.0 | 94.5 | 40.0 | 93.8 |
Swede score ≥ 5 | 74.1 | 45 | 11.8 | 94.6 |
Swede score ≥ 8 | 11.1 | 92.3 | 12.5 | 91.3 |
Test | Sensitivity (%) | Specificity (%) | Positive predictive value (%) | Negative predictive value (%) |
Reid’s score ≥ 5 | 37.0 | 94.5 | 40.0 | 93.8 |
Swede score ≥ 5 | 74.1 | 45 | 11.8 | 94.6 |
Swede score ≥ 8 | 11.1 | 92.3 | 12.5 | 91.3 |
Narakas classification | Total 200 (100%) | Grade 1 72 (36%) | Grade 2 64 (32%) | Grade 3 50 (25%) | Grade 4 14 (7%) |
Complete recoverya | 107 (54) | 60 (83) | 40 (63) | 7 (14) | - |
Near complete functional recovery but partial deformitya | 22 (11) | 5 (7) | 10 (16) | 6 (12) | 1 (7) |
Partial recovery with gross functional defect and deformity | 31 (16) | 7 (10) | 13 (20) | 10 (20) | 1 (7) |
No significant improvement | 40 (20) | - | 1 (1.5) | 27 (54) | 12 (86) |
aSatisfactory recovery bGrade 1, C5, 6, 7 improvement; Grade 2, C5, 6, 7 improvement; Grade 3, panpalsy C5, 6, 7, 8, 9, Grade 4, panpalsy with Hornon’s syndrome. | |||||
Narakas classification | Total 200 (100%) | Grade-1 72 (36%) | Grade-2 64 (32%) | Grade-3 50 (25%) | Grade-4 14 (7%) |
Complete recoverya | 107 (54) | 60 (83) | 40 (63) | 7 (14) | - |
Near complete functional recovery but partial deformitya | 22 (11) | 5 (7) | 10 (16) | 6 (12) | 1 (7) |
Partial recovery with gross functional defect and deformity | 31 (16) | 7 (10) | 13 (20) | 10 (20) | 1 (7) |
No significant improvement | 40 (20) | - | 1 (1.5) | 27 (54) | 12 (86) |
aSatisfactory recovery bGrade 1, C5, 6, 7 improvement; Grade 2, C5, 6, 7 improvement; Grade 3, panpalsy C5, 6, 7,8,9, Grade 4, panpalsy with Hornon’s syndrome. | |||||
Variables in probe trial day | Groups | ||||
NC | SC | ColC | Pre-SwE Exp | Post-SwE Exp | |
Target crossings | 8.0 (0.3) | 7.3 (0.3) | 1.7 (0.2)a | 6.0 (0.3)a | 5.8 (0.4)a |
Time spent in target | 18.0 (0.4) | 16.2 (0.7) | 5.8 (0.8)a | 15.3 (0.7)a | 15.2 (0.9)a |
NC indicates normal control; SC, Sham control; ColC, colchicine control; SwE, swimming exercise exposure. aP <0.01. | |||||
Pain level | Number (%) | P | ||
Pre | Post 1 | Post 2 | ||
Mean (SD)a pain score | 4.7 (1.9) | 2.7 (1.6) | 0.8 (1.1) | <0.001 |
Pain categories | ||||
No pain (0) | - | 1 (1.7) | 31 (51.7) | <0.001 |
Mild pain (1-3) | 15 (25.0) | 43 (70.0) | 27 (45.0) | |
Moderete pain (4-6) | 37 (61.7) | 15 (25.0) | 2 (3.3) | |
Severe pain (7-10) | 8 (13.3) | 2 (3.3) | - | |
aPain scores according to the visual analogue scale ranging from 0 to 10; SD indicates standard deviation | ||||
Surgeries | Number (%) | Satisfactory outcomes n (%) |
Primary surgery (n=24) |
|
|
Upper plexus | 6 (25) | 5 (83) |
Pan-palsy | 18 (75) | 6 (33) |
All | 24 (100) | 11 (46) |
Secondary Surgery (n=26) |
|
|
Shoulder deformity | 15 (58) | 13 (87) |
Wrist and forearm deformity | 11 (42) | 6 (54) |
All | 26 (100) | 19 (73) |
Primary and secondary surgery | 50 (100) | 30 (60) |
Mallet score 14 to 25 or Raimondi score 2-3 or Medical Research grading >3 to 5. | ||
Narakas classification | Total 200 (100%) | Grade-1 72 (36%) | Grade-2 64 (32%) | Grade-3 50 (25%) | Grade-4 14 (7%) |
Complete recoverya | 107 (54) | 60 (83) | 40 (63) | 7 (14) | - |
Near complete functional recovery but partial deformitya | 22 (11) | 5 (7) | 10 (16) | 6 (12) | 1 (7) |
Partial recovery with gross functional defect and deformity | 31 (16) | 7 (10) | 13 (20) | 10 (20) | 1 (7) |
No significant improvement | 40 (20) | - | 1 (1.5) | 27 (54) | 12 (86) |
aSatisfactory recovery bGrade 1, C5, 6, 7 improvement; Grade 2, C5, 6, 7 improvement; Grade 3, panpalsy C5, 6, 7,8,9, Grade 4, panpalsy with Hornon’s syndrome. | |||||
Trials | Groups | ||||
NC | SC | ColC | Pre-SwE Exp | Post-SwE Exp | |
1 | 20.8 (0.6) | 22.1 (1.8) | 41.1 (1.3)b | 31.9 (1.9)b | 32.9 (1.8)a, b |
2 | 10.9 (0.6) | 14.9 (1.7) | 37.4 (1.1)b | 24.9 (2.0)b | 26.8 (2.5)b |
3 | 8.4 (0.5) | 9.9 (2.0) | 32.8 (1.2)b | 22.0 (1.4)b | 21.0 (1.4)b |
4 | 7.8 (0.5) | 10.4 (1.3) | 27.6(1.1)b | 12.8 (1.2)b | 13.0 (1.4)b |
Savings (%)c | 47.7 (3.0) | 33.0 (3.0) | 10.0 (0.9)b | 23.6 (2.7)b | 18.9 (5.3)b |
NC indicates normal control; SC, Sham control; ColC, colchicine control; SwE, swimming exercise exposure. aP <0.05; bP <0.01. cThe difference in latency scores between trials 1 and 2, expressed as the percentage of savings increased from trial 1 to trial 2 | |||||


Lesion-size | Histopathology report | Total | |||||
CIN1 | CIN2 | CIN3 | ICC | CC | SM | ||
0–5 mm | 73 | 0 | 0 | 0 | 5 | 5 | 83 |
6–15 mm | 119 | 18 | 1 | 4 | 0 | 0 | 142 |
>15 mm | 1 | 8 | 31 | 23 | 12 | 0 | 75 |
Total | 193 | 26 | 32 | 27 | 17 | 5 | 300 |
CIN indicates cervical intraepithelial neoplasia; ICC, invasive cervical cancer; CC, chronic cervicitis; SM, squamous metaplasia | |||||||
| Histopathology report | Total | ||||||
CIN1 | CIN2 | CIN3 | ICC | CC | SM | |||
Lesion -Size | 0-5 mm | 73 | 0 | 0 | 0 | 5 | 5 | 83 |
6-15 mm | 119 | 18 | 1 | 4 | 0 | 0 | 142 | |
>15 mm | 1 | 8 | 31 | 23 | 12 | 0 | 75 | |
Total | 193 | 26 | 32 | 27 | 17 | 5 | 300 | |
CIN indicates Cervical intraepithelial neoplasia; ICC, Invasive cervical cancer; CC, Chronic cervicitis; SM, Squamous metaplasia | ||||||||
Group | Didactic posttest marks (%) | Flipped posttest marks (%) | Difference in marks (mean improvement) | P |
<50% | 63.2 (9.4) | 82.2 (10.8) | 19.0 | <0.001 |
≥50% | 72.4 (14.9) | 84.2 ( 10.3) | 11.8 | <0.001 |
Data presented as mean (standard deviation) | ||||








